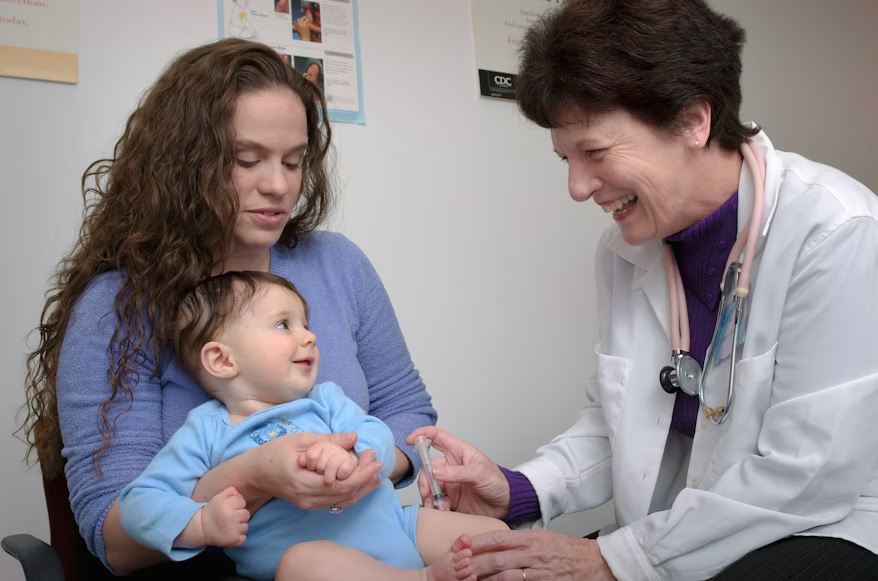
The 12-week vaccine visit is a milestone most new parents dread a little. The baby gets several shots at once, and within hours the household can shift from calm to chaotic: low-grade fever, inconsolable crying, a swollen thigh, and nobody sleeping. For families where one or both parents work overnight or irregular shifts, the timing can feel impossible. Here is what pediatricians and public health agencies actually say about post-vaccine reactions at this age, when to worry, and how to plan so the whole family survives the next 48 hours.
What vaccines does a 12-week-old receive?
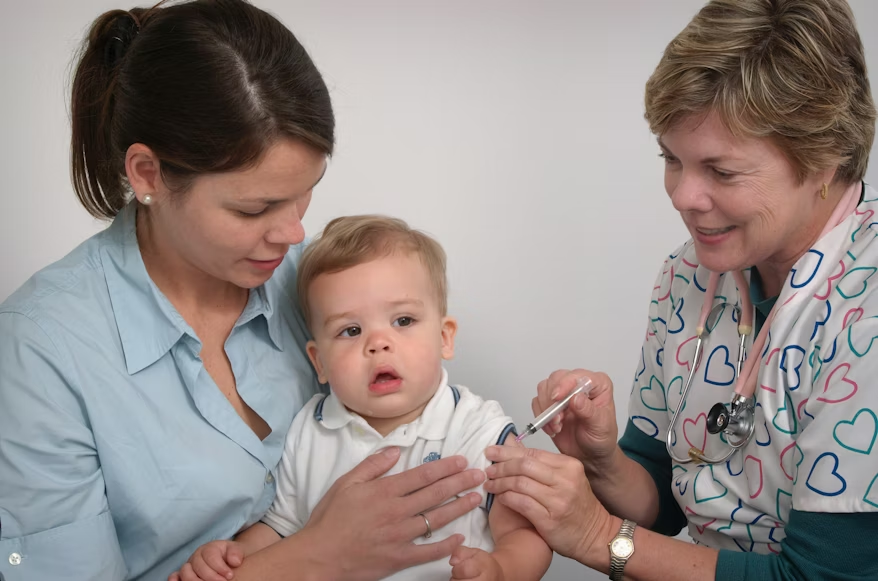
According to the CDC’s recommended immunization schedule, babies at the two-month visit (often given between 8 and 12 weeks) typically receive doses of DTaP (diphtheria, tetanus, pertussis), inactivated polio (IPV), Haemophilus influenzae type b (Hib), pneumococcal conjugate (PCV15 or PCV20), rotavirus (oral), and hepatitis B. That can mean three or four injections plus an oral dose in a single appointment. Each vaccine triggers a separate immune response, which is why the hours and days afterward can be rougher than parents expect.
Normal side effects and how long they last
Short-term reactions are common and, in most cases, a sign the immune system is doing exactly what it should. The CDC’s guide to possible side effects lists soreness or swelling at the injection site, low-grade fever, fussiness, and sleepiness as the most frequent responses. These typically appear within 6 to 12 hours of the shots and resolve within 48 hours.
A baby at this age has limited ways to communicate discomfort. Increased crying, shorter feeding sessions, and disrupted sleep are all normal expressions of the mild inflammation vaccines produce. The American Academy of Pediatrics (AAP) advises that infant acetaminophen (Tylenol) can be given to babies three months and older to manage pain and fever, dosed by weight rather than age. Parents should confirm the correct dose with their pediatrician before vaccine day so the medication is ready at home.
One concern that circulates online is whether giving acetaminophen before or right after shots might blunt the immune response. A 2009 study in The Lancet raised that question, but subsequent research, including a review published in Pediatrics, found no clinically significant reduction in antibody levels when acetaminophen was used for symptom relief after vaccination. The current AAP position: treat discomfort as needed.
When to call the pediatrician or go to the ER
Most post-vaccine symptoms are self-limiting, but a small number of reactions require prompt medical attention. The CDC notes that serious problems after vaccination happen much less often than mild ones, but parents should know the red flags:
- Fever above 104°F (40°C), or any fever in a baby under 8 weeks old
- Crying that lasts more than three hours and cannot be consoled
- Limpness, unusual floppiness, or decreased responsiveness
- Difficulty breathing, wheezing, or swelling of the face and throat (signs of a rare allergic reaction)
- A rash that spreads rapidly or looks like hives
Severe allergic reactions (anaphylaxis) almost always occur within 15 to 30 minutes of the injection, which is one reason pediatric offices ask families to wait in the clinic after shots. If any of the symptoms above appear at home, parents should call 911 (or their local emergency number) rather than drive to the ER themselves.
Why the 12-week mark feels especially hard
At roughly three months, a baby is gaining neck and trunk strength but is still far from sitting independently, let alone standing. The CDC’s developmental milestones tracker notes that a two-month-old can hold their head up briefly during tummy time and may push up on arms while on their stomach. When post-vaccine soreness or fever makes a baby suddenly floppier or less interested in feeding, it can look alarming. But the change parents are seeing is usually discomfort, not a developmental regression. If a baby returns to baseline behavior within two to three days, there is generally no cause for concern.
This period also coincides with the tail end of the “fourth trimester,” when many parents are still adjusting to fragmented sleep. Adding a fussy, feverish baby to an already sleep-deprived household can push caregivers to a breaking point, especially those working night shifts or jobs with irregular hours.
Managing vaccine day when a parent works nights
Shift work and infant care are a notoriously difficult combination. A 2018 report in Pediatrics found that parental sleep disruption in the first year is associated with increased stress, impaired decision-making, and higher rates of postpartum mood disorders. Layering a rough vaccine night on top of chronic sleep debt raises real safety concerns, particularly for parents who drive, operate machinery, or provide patient care during overnight shifts.
Practical steps that pediatricians and occupational health experts recommend:
- Schedule vaccines before a day off. If one parent works nights, book the appointment so the hardest 24 to 48 hours fall on that parent’s off days.
- Prepare a comfort station. Set out acetaminophen (with the correct dose written down), a digital thermometer, cool washcloths, and a phone with the pediatrician’s after-hours number saved.
- Split the night in shifts. One caregiver handles the first four hours post-bedtime; the other takes over for the second half. Even partial uninterrupted sleep blocks are more restorative than constant waking.
- Line up backup. A grandparent, neighbor, or postpartum doula who can hold the baby for a few hours the next day lets the overnight caregiver recover safely.
- Communicate with your employer. Some workplaces offer shift swaps or short-notice personal days. Asking in advance is easier than calling out at midnight.
Preparing for the next round
The two-month vaccines are just the beginning. The CDC schedule calls for another set of doses at four months and again at six months, with additional boosters through toddlerhood. Each round can bring similar side effects, though many parents report that reactions become more predictable and less anxiety-inducing over time.
Keeping a simple log helps. After each appointment, note which vaccines were given, what symptoms appeared, how long they lasted, and what helped. That record gives the pediatrician useful information and gives parents a reference point: “Last time the fussiness peaked at eight hours and was gone by morning” is far more reassuring than trying to remember through a fog of sleep deprivation.
The science is clear that the short-term discomfort of vaccination is vastly outweighed by the protection it provides against diseases like pertussis, which hospitalized more than 1,100 infants under 12 months in the United States in a single recent season, according to CDC surveillance data. Knowing that context does not make a feverish 3 a.m. any easier, but it can steady a parent’s resolve when the next appointment rolls around.
More from Decluttering Mom: