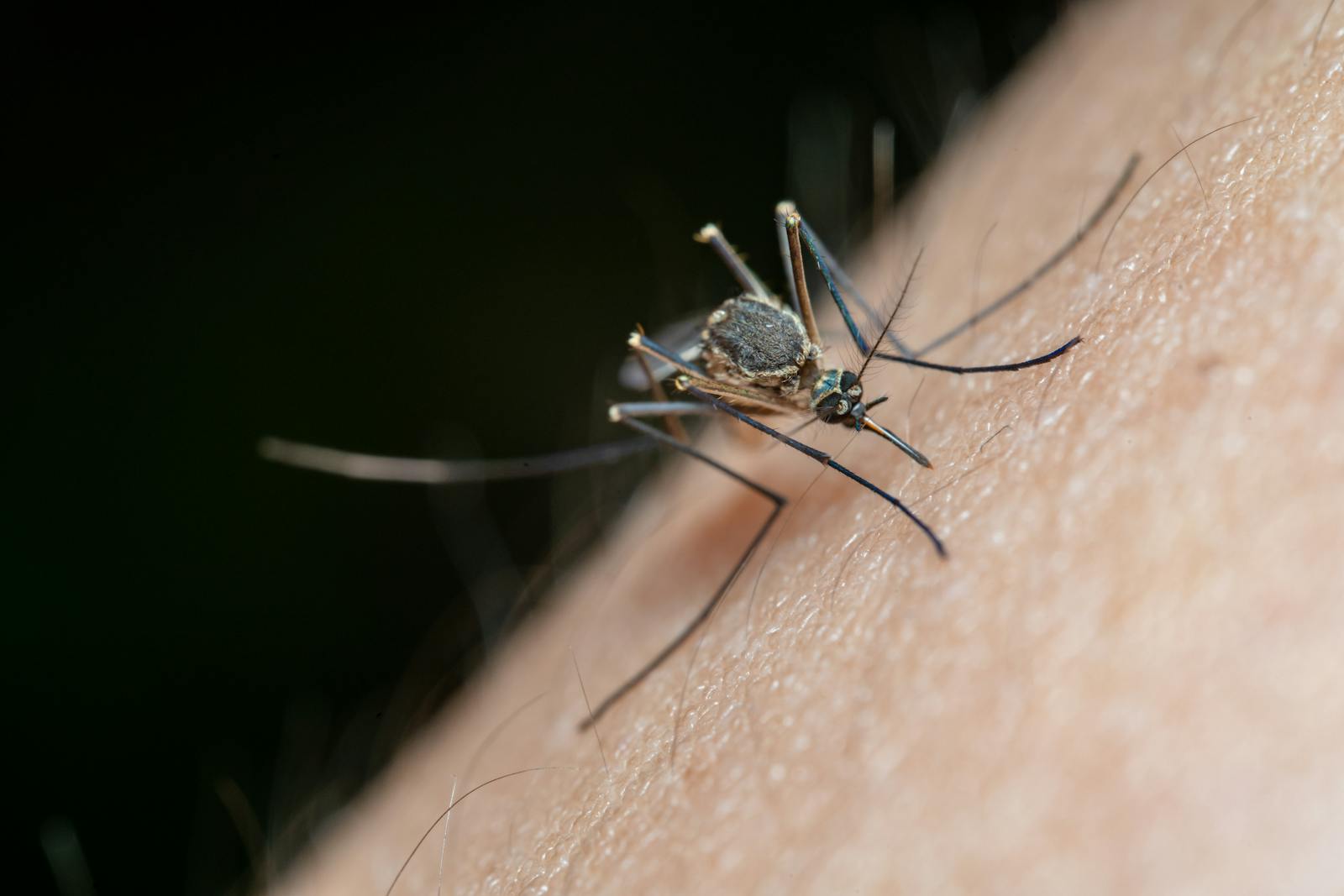
You’re likely to notice more mosquitoes this season, and that matters because several species that carry dangerous viruses are expanding their range and season. Health officials urge taking simple steps now to reduce bites, monitor symptoms, and protect vulnerable people so small actions can prevent serious illness.
Take immediate, practical precautions—eliminate standing water, use EPA-registered repellents, and secure window screens—to lower your chance of infection as mosquito activity increases.
They will explain which mosquito species are spreading, which diseases to watch for, and exactly how to prepare your home and family so you’re ready if local transmission rises.
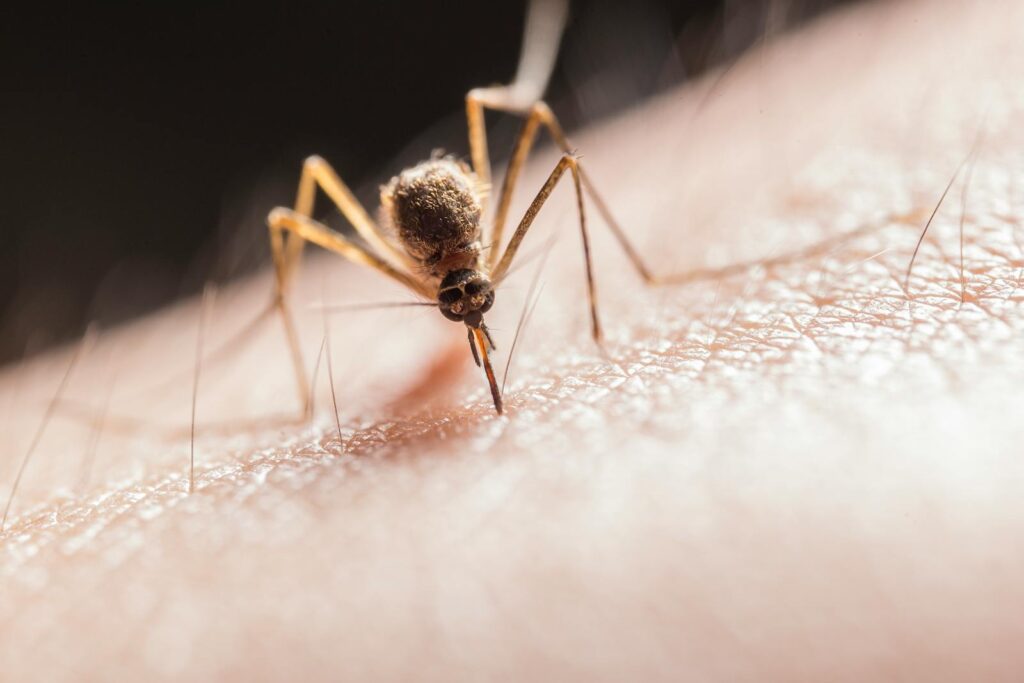
Health Experts Warn About a Surge of the World’s Deadliest Mosquito Species
Health officials note rising numbers of mosquito-borne illnesses, expanding mosquito ranges, and gaps in surveillance and control that leave many U.S. communities vulnerable. They emphasize targeted prevention, stronger local entomology capacity, and public awareness to reduce transmission risk.
Why Mosquitoes are Called the World’s Deadliest Animal
Mosquitoes transmit multiple pathogens that cause high illness and death rates: malaria parasites, dengue, Zika, chikungunya, yellow fever, and West Nile virus. The CDC documents how these vectors produce recurring outbreaks, overwhelm local clinics, and cause long-term disability in affected populations.
Transmission depends on species. Aedes aegypti and Aedes albopictus efficiently spread dengue, Zika, chikungunya, and yellow fever in urban and peri-urban settings. Anopheles stephensi and other Anopheles species transmit malaria and have expanded into new regions, increasing local risk.
Public health impact includes seasonal spikes in emergency visits, pregnancy complications with Zika, and neurological outcomes from West Nile and chikungunya. The World Health Organization tracks global trends and recommends vaccination and vector control where feasible.
Surging Mosquito Populations: What’s Driving the Risk?
Mosquito breeding increases where standing water collects: clogged gutters, tires, storm drains, and containers in yards. Urban environments with poor drainage and dense human populations create ideal conditions for Aedes species to amplify transmission quickly.
Human travel and trade move mosquitoes and viruses across borders. Used tires, shipping containers, and air travel have introduced Aedes albopictus and Aedes aegypti into new regions in past decades, leading to local outbreaks in places previously free of those pathogens.
Public health systems face reduced entomology staffing and surveillance capacity, limiting early detection of new introductions. Experts urge rebuilding state and local mosquito-control programs and expanding laboratory testing to catch transmission earlier and guide targeted interventions.
Climate Change, Urbanization, and Mosquito Expansion
Warming trends lengthen mosquito season and raise survival rates for larvae and adult vectors. Warmer nights and earlier springs allow faster viral replication inside mosquitoes, shortening the time to infectiousness and increasing transmission potential.
Urbanization creates heat islands and water-holding infrastructure that favor Aedes aegypti, which breeds in small artificial containers close to humans. Rapid population growth in tropical and subtropical cities further magnifies contact between people and vectors.
Climate-driven range shifts have allowed Anopheles stephensi and other species to colonize areas that were once too cool. Public health authorities, including the CDC, warn that without enhanced surveillance and urban planning changes, more U.S. regions could see local transmission of dengue, malaria, and other vector-borne diseases.
- Key actions recommended: restore entomology staffing, improve stormwater management, remove standing-water habitats, and expand community education programs.
- Technical tools: targeted insecticide application, larval source management, and genomic surveillance to detect introductions early.
Risks From Mosquito-Borne Diseases and How to Prepare
Mosquito-borne diseases can cause everything from short fevers to life‑threatening illness. Individuals should know which viruses and parasites are circulating locally, how infections are diagnosed, and what simple steps cut exposure and community risk.
Current and Emerging Diseases: Dengue, Malaria, and More
Dengue causes high fever, severe headache, rash, and intense joint and muscle pain often called “break‑bone fever.” Severe dengue can lead to bleeding and shock and requires urgent care. Recent years have seen more reports of locally acquired dengue in parts of the U.S. and territories; travelers can also bring infections home.
Malaria, caused by Plasmodium parasites, produces cyclical fevers and chills and can become fatal without prompt treatment. Most U.S. malaria cases follow international travel, but climate and vector changes raise outbreak risk where Anopheles mosquitoes persist.
West Nile virus often causes mild fever but can progress to neurological disease in older adults. Zika and chikungunya produce fever, rash, and joint pain; Zika also risks congenital harm in pregnancy. Eastern equine encephalitis (EEE) is rare but has high fatality and severe neurologic outcomes.
How Mosquitoes Spread Diseases and Impact Public Health
Mosquitoes pick up pathogens when they bite infected humans or animals, then transmit them during later bites. Different species carry different pathogens: Aedes aegypti and Aedes albopictus transmit dengue, Zika, and chikungunya; Culex species commonly transmit West Nile virus; Anopheles species transmit malaria.
Surveillance and diagnostic tests identify cases and guide responses. Public health agencies, including the Centers for Disease Control and Prevention, track mosquito populations and human cases to detect outbreaks early. Increased travel, warmer temperatures, and standing or stagnant water that breeds mosquitoes expand range and season, amplifying community risk. Vector-borne disease burdens strain hospitals and require targeted mosquito control and public communication.
Staying Safe: Preventing Mosquito Bites and Reducing Risk
Wear long sleeves and long pants treated with permethrin when in mosquito‑dense areas. Apply EPA-registered repellents containing DEET, picaridin, IR3535, or oil of lemon eucalyptus to exposed skin per label instructions; these work for adults, pregnant and breastfeeding people when used as directed.
Eliminate breeding sites by draining or treating standing water in gutters, flower pots, bird baths, and tires every 3–7 days. Use window and door screens or air conditioning and sleep under nets where indoor protection is limited. After travel to areas with dengue, Zika, or chikungunya, avoid mosquito exposure for three weeks to reduce risk of local transmission.
Community and Public Health Measures Americans Should Know
Public health partners coordinate mosquito control programs that include larval habitat removal, targeted insecticide spraying, and community education. Local health departments perform surveillance—trapping mosquitoes and testing pools for West Nile, EEE, and other mosquito-borne viruses—and report findings to regional centers and the CDC.
Residents should report unusual mosquito abundance or clusters of febrile illness to local health authorities and get tested if symptoms like fever, rash, severe joint pain, or neurologic signs develop after mosquito exposure. Health systems rely on timely diagnostic tests to confirm dengue, malaria, or other infections and to trigger vector control and contact‑tracing measures.
More from Decluttering Mom: