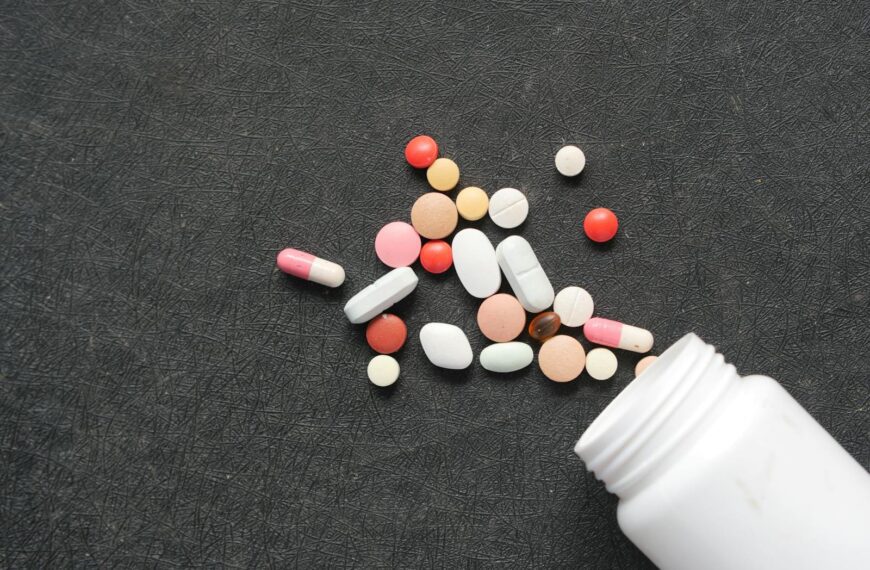
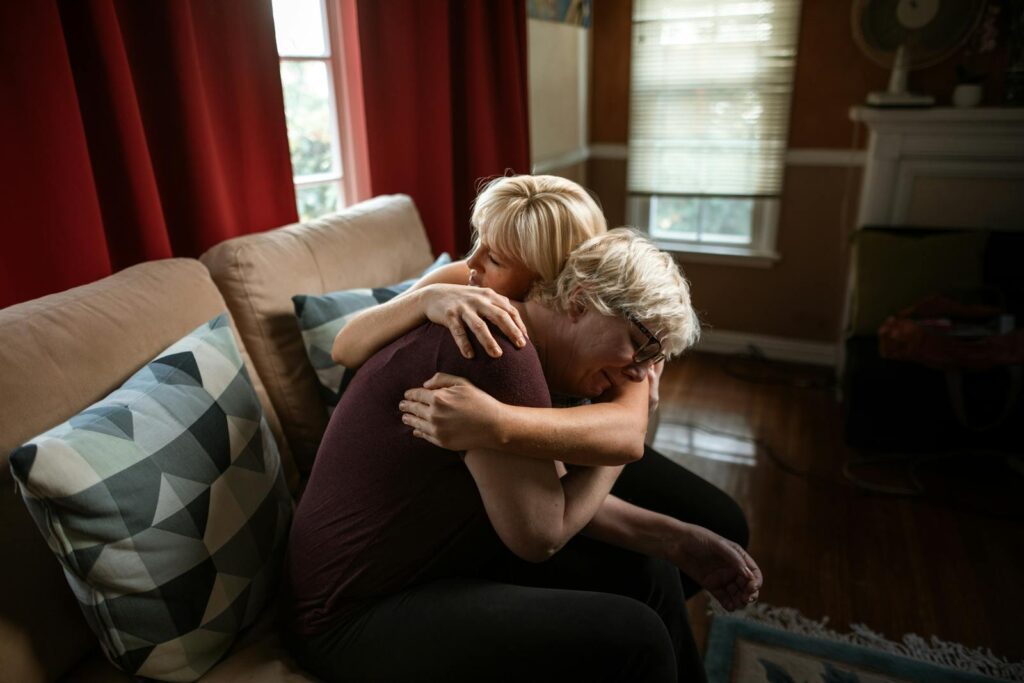She had imagined the first months with her third baby would feel familiar. Instead, a mother of three recently described the experience in a parenting forum with a word that stopped other parents mid-scroll: “luggage.” The newborn, she wrote, was strapped into a car seat and shuttled from school drop-off to soccer practice to the grocery store, rarely the reason for any trip, always just along for the ride. Dozens of replies echoed the same guilt: I felt that too, and I was afraid to say it out loud.
That guilt is worth unpacking, because the feeling is far more common than most new parents realize, and its roots are less about individual shortcomings than about the way American work schedules, family logistics, and parental leave policies collide during the most vulnerable stretch of early parenthood.
Back at work before the fourth trimester ends

By the time a baby is 12 weeks old, a striking number of American mothers have already returned to their jobs. A 2020 analysis published in the Journal of Women’s Health found that 55 percent of U.S. women return to work during their child’s infancy, with the majority doing so within the first three months after delivery. The United States remains the only wealthy nation that does not guarantee paid parental leave at the federal level; the Family and Medical Leave Act provides up to 12 weeks of unpaid, job-protected leave, but only for workers who meet eligibility requirements, which the Department of Labor estimates excludes roughly 44 percent of the workforce.
That policy gap means many parents are still healing from childbirth, still learning a newborn’s cues, and still waking every two to three hours at night when they sit back down at a desk and try to perform as though nothing has changed. Behavioral health researchers at the University of Rochester Medical Center describe this reentry window as a period of acute vulnerability, noting that for some parents, returning to work feels like a relief and a reconnection to a familiar identity, while for others it triggers a rush of anxiety, grief, and a nagging sense that they are failing on every front simultaneously.
When bonding feels mechanical
The “luggage” metaphor is blunt, but therapists who specialize in postpartum mental health say it captures something real: emotional blunting under sustained overload. When a parent is toggling between a client call, a school pickup, and a diaper change in a parking lot, caregiving can start to feel like task management rather than connection.
That numbness is not evidence of being a bad parent. The American College of Obstetricians and Gynecologists notes that postpartum depression affects roughly 1 in 7 women and can include feelings of emotional distance from the baby, difficulty concentrating, and a persistent sense of being overwhelmed. Postpartum anxiety, which often co-occurs, can make even routine caregiving feel frantic and joyless. Both conditions are treatable, and clinicians stress that parents do not need to wait until they are in crisis to seek help. Postpartum Support International operates a free helpline (1-800-944-4773) and a crisis text line (text “HELP” to 988) for parents who need immediate support.
Fathers and non-birthing partners are not immune. Research published in JAMA Psychiatry has found that roughly 8 to 10 percent of fathers experience depression in the first year after a child’s birth, a rate that climbs when sleep deprivation and financial stress are high. The “luggage” feeling can land on any parent carrying too much with too little support.
The second-child schedule trap
First-time parents typically build their days around the baby: nap windows dictate errands, feeding times override dinner reservations, and the household bends to accommodate a seven-pound newcomer. With a second or third child, that dynamic often inverts. School start times, sports practices, and homework routines are already locked in, and the newborn is expected to fit around them.
Maida Lynn Chen, director of the Pediatric Sleep Disorders Center at Seattle Children’s Hospital, has urged parents in this situation to “respect the naps” and protect at least some predictable sleep periods for the infant, even when older children’s schedules are demanding. Without that protection, the baby’s biological needs are constantly overridden, which can deepen a parent’s sense that the infant is just cargo being moved from one stop to the next.
The logistical crunch is real, but so is the emotional cost. When a newborn never gets to be the reason the family slows down, the parent-infant relationship can feel like it is developing in the margins, squeezed into whatever minutes are left after everyone else’s needs have been met.
Sleep deprivation makes everything worse
No discussion of early parenthood is complete without confronting sleep loss, which functions as a threat multiplier for every other stressor on this list. Newborns wake every two to three hours to feed, and that fragmented sleep pattern collides directly with the cognitive demands of paid work and the physical demands of managing a household with older children.
The Centers for Disease Control and Prevention classifies insufficient sleep as a public health concern, and research consistently links chronic sleep deprivation to impaired emotional regulation, reduced empathy, and difficulty forming new memories. For a new parent, that translates into a flattened capacity to feel joy, patience, or connection, exactly the emotional resources that bonding with an infant requires. A parent running on four hours of broken sleep is not choosing to feel detached; their brain is operating in survival mode.
What real support looks like
Structural problems require structural solutions, but individual families cannot wait for federal paid-leave legislation to pass. In the meantime, several strategies can help parents reclaim a sense of connection with a new baby even inside a packed schedule.
Negotiate the return. Workplace guidance from Bright Horizons encourages parents to communicate openly with supervisors about a phased reentry: starting with reduced hours, setting short-term goals, and acknowledging that the transition will take time. Not every employer will accommodate this, but asking is a first step, and documenting the request creates a record.
Protect small pockets of one-on-one time. Bonding does not require hours of uninterrupted togetherness. Even brief, focused moments matter. A quiet cuddle before the older children wake up, or five minutes of skin-to-skin contact after the evening rush, can remind a parent that this is a relationship, not a logistics problem. Some parenting educators recommend structured micro-rituals, such as spending seven dedicated, device-free minutes with each child in the morning, after work, and before bed, as a way to build presence without adding hours of new obligations.
Name the feeling without judging it. Telling yourself “I feel like my baby is luggage” is not a confession of failure. It is information. It signals that the current setup is not sustainable and that something, whether it is workload, sleep, mental health support, or help at home, needs to change. Therapists who work with postpartum families consistently say that acknowledging the feeling is the first step toward addressing it.
Screen for postpartum mood disorders early. ACOG recommends that clinicians screen for depression and anxiety at least once during the perinatal period, but parents can also self-screen using validated tools like the Edinburgh Postnatal Depression Scale, available free through Postpartum Support International. A score that raises concern is a reason to call a provider, not a reason to push through alone.
The feeling that a new baby is “just along for the ride” is painful, but it is also a signal that can be read and acted on. Most parents who get adequate sleep, reasonable work accommodations, and timely mental health support find that the sense of detachment lifts and that bonding catches up. The baby was never really luggage. The parent was just carrying too much of everything else.
More from Decluttering Mom: